
Feb 15, 2026 | Healthy Tips

How diabetes and cancer are linked, why cancer survivors face diabetes risk, and what new-onset diabetes may reveal about hidden cancers.
By Justine Evans
Some facts about diabetes and cancer:
- Type 2 diabetes increases risk for certain cancers.
- Some cancer treatments may cause diabetes later.
- New-onset diabetes in older adults may signal hidden cancer.
- Screening and lifestyle changes can reduce risk.
- Research is exploring new diagnostic tools using these links.
If you’re living with diabetes, you might know all about the intriguing and intricate relationship between diabetes and certain types of cancer. And it’s not a one-way street — the connection goes both ways.
So, what does current research say about this bidirectional relationship? Why are some cancer survivors more likely to develop diabetes? And why is understanding the difference between new-onset and long-standing diabetes critical in cancer detection and care?
Which cancers are linked to diabetes?
It’s been known for some time that diabetes, especially type 2 diabetes, can increase the risk of several types of cancer. But which cancers specifically?
According to a growing body of evidence, people with diabetes are more likely to develop pancreatic, liver, colorectal, breast and endometrial cancers. Why these cancers in particular? Different factors may be at play:
- People with type 2 diabetes often have higher circulating insulin levels, which may promote the growth of cancer cells.
- Long-term low-grade inflammation, common in diabetes, can create an environment in the body that’s more vulnerable to cancer development.
- Persistently high glucose levels may not only damage blood vessels and organs but also contribute to tumour growth.
A 2025 review in Seminars in Oncology outlines these mechanisms in detail, underscoring that this isn’t just correlation butthe risk that there’s a plausible biological basis linking diabetes to cancer risk.
It’s been known for some time that diabetes, especially type 2 diabetes, can increase the risk of several types of cancer. But which cancers specifically?
The gender gap in diabetes-related cancer risk
Diabetes doesn’t affect everyone’s cancer risk in the same way. In fact, research shows that women with diabetes tend to have a higher overall risk of developing cancer than men with diabetes. Across many different cancer types, the relative increase in cancer risk associated with diabetes was greater in women. Importantly, this wasn’t limited to a single cancer. Instead, diabetes appeared to place a broader cancer burden on women overall.
So why might this difference exist? The answer is likely complex and involves a mix of biological and lifestyle factors. Many of the risk factors shared by diabetes and cancer, such as excess body weight, physical inactivity and smoking, can worsen insulin resistance and promote long-term inflammation in the body.
These changes can also disrupt hormone regulation, all of which are processes linked to cancer development. Some evidence suggests that these metabolic and lifestyle effects may be more pronounced, or persist for longer, in women with diabetes. Over time, this may help explain why women experience a greater relative increase in cancer risk compared with men, even when both are living with the same condition.
Can cancer treatments cause diabetes?
Interestingly, the relationship works the other way, too. People who have survived cancer, particularly those treated with certain therapies, are at greater risk of developing new-onset diabetes after cancer.
A recent article published in Annals of Medicine and Surgery (2024) explored how cancer treatments, while life-saving, can disrupt glucose metabolism in various ways. Here are a few examples:
- Chemotherapy and corticosteroids, often used to manage cancer or treatment side effects, can cause spikes in blood sugar.
• Androgen deprivation therapy (used in prostate cancer) has been associated with insulin resistance.
• Abdominal radiation, particularly in children and young adults, can damage the pancreas, impairing insulin production.
This risk is beyond a simple short-term issue during treatment. For many survivors, diabetes may not appear until months or even years later. And because cancer follow-up typically focuses on recurrence and surveillance imaging, blood glucose levels might not be closely monitored unless there’s a specific concern.
People who have survived cancer, particularly those treated with certain therapies, are at greater risk of developing new-onset diabetes after cancer
It’s not just a case of better detection
You might ask whether there is simply an increase in diabetes and cancer diagnoses because we’re looking more closely. After all, both conditions are common, and frequent medical visits often lead to more testing. But experts now agree this is more than just detection bias. A growing number of studies demonstrate a biologically plausible connection between the two conditions.
For instance, shared risk factors, such as obesity, sedentary lifestyle, poor diet, and inflammation, as well as treatment-related effects that support this real, bidirectional link. Although these shared risk factors present a more complex picture, the association between diabetes and certain cancers remains.
That means clinicians are not just diagnosing more people by chance. There is a real link that has clinical implications for diabetes management and cancer care.
New-onset vs long-standing diabetes: a new focus in research
Here’s where it gets even more interesting. Researchers are now focused on distinguishing new-onset diabetes, especially in older adults, as a potential early marker of underlying cancer, particularly pancreatic cancer.
Why pancreatic cancer? Because in many cases, new-onset diabetes can precede the cancer diagnosis. The pancreas is central to both insulin production and tumour development, and a pancreatic tumour can impair insulin secretion, sometimes months before the cancer is detected.
So, while long-standing diabetes may increase the risk of developing certain cancers over time, sudden-onset diabetes, especially in someone with no history of obesity or insulin resistance, could be a red flag. This is especially important because pancreatic cancer often presents late and has poor survival outcomes. Early detection can make a big difference.
In fact, healthcare systems are exploring screening programmes that use new-onset diabetes in people over 50 as a trigger to investigate for pancreatic cancer. It’s a promising area of research that could lead to earlier diagnoses and better outcomes.
Sudden-onset diabetes, especially in someone with no history of obesity or insulin resistance, could be a red flag
What does this mean for people living with diabetes or cancer?
Understanding this bidirectional relationship matters for individuals and healthcare providers.
- If you have diabetes: Regular cancer screenings, especially for colorectal, breast, and liver cancers, may be more relevant than ever. Maintaining good glycaemic control, staying active and managing weight could help reduce your risk.
- If you’re a cancer survivor: Keep an eye on your blood glucose levels, even years after treatment. If you were exposed to chemotherapy, steroids, radiation, or hormone therapy, you may have a higher chance of developing diabetes, and early diagnosis is key.
- If you’re newly diagnosed with diabetes in your 50s or older: Talk to your GP about whether further investigation might be needed, particularly if you don’t fit the type 2 diabetes profile. It might be nothing, but it’s worth checking.
What’s next in research?
The complex interaction between diabetes and cancer is now one of the most dynamic areas of medical research. With a better understanding, there’s hope that:
- Cancer therapies are refined to reduce metabolic side effects.
- New-onset diabetes can serve as a valuable biomarker for early cancer detection.
- Strategies are developed to prevent diabetes in cancer survivors through tailored screening and lifestyle support.
It’s a reminder that in medicine, everything is connected, and sometimes the clues to one condition or disease lie in the symptoms or progression of another.
In medicine, everything is connected, and sometimes the clues to one condition or disease lie in the symptoms or progression of another.
Should people with diabetes be alarmed?
Living with diabetes doesn’t mean you’re destined to develop cancer, and not all cancer survivors will go on to develop diabetes. But recognising the links between these conditions can empower you to take preventive action, ask informed questions, and work with your healthcare team for more personalised care.
After all, the more we understand how diseases interact, the better we can treat and prevent them.
https://diabetesvoice.org/en/caring-for-diabetes/diabetes-and-cancer-whats-the-real-connection/?mc_cid=0daf1860af&mc_eid=50b74717d8

Feb 14, 2026 | Healthy Tips
Anita Sabidi

The myth of the supermom: embracing vulnerability with Type 1 Diabetes
Motherhood is often painted as a story of strength, resilience, and endless sacrifice. As mothers, we are expected to be the pillars of our families—the ones who hold everything together no matter what. But living with Type 1 diabetes for more than two decades has taught me that being a mother does not mean being invincible. In fact, one of the most valuable lessons I’ve been able to share with my children is that their mama is not a superwoman. I can be strong, yes, but I can also be vulnerable. And that’s okay.
Type 1 Diabetes is a family affair: when daily rituals become childhood memories
Every day with diabetes is a balancing act. Managing insulin, blood sugar checks, and the unpredictability of the condition can feel like carrying an invisible load. Yet this journey is not mine alone—it has become a family affair. My children have grown up witnessing my daily rituals with insulin injections and blood glucose monitoring. What might seem routine to me is part of their childhood memories, shaping how they understand care, responsibility, and empathy.
“Cover mama!”: how my kids became my little bodyguards
One of the sweetest moments happens whenever it’s time for my insulin shot in public. Without being asked, my kids instinctively take position around me, shielding me from curious stares. “Cover Mama!” they say, forming a protective circle as I inject. In those little moments, I see their love, their awareness, and their willingness to step into the role of supporters. They are my little bodyguards, and I treasure that more than words can describe.
Why sharing my needs is a lesson in strength, not a burden
Some might think children shouldn’t have to carry that kind of responsibility. But I see it differently. By sharing my vulnerabilities with them, I am teaching them important lessons about life: that strength is not about pretending to be unbreakable, but about acknowledging our needs and asking for support. That caring for one another is not a burden, but an act of love.
Authenticity over perfection: what my children taught me about Type 1 Diabetes resilience
Motherhood with diabetes has also shown me that I don’t have to live up to the impossible standard of being a superwoman. My kids don’t need perfection; they need authenticity. They need to see that it’s human to struggle, to adapt, and to keep going despite the challenges. They need to know that resilience comes not from denying vulnerability, but from embracing it.
So yes, I am a mother living with diabetes. I am a caregiver, but I am also someone who needs care. And in this shared journey, my children and I are learning together—that family is not about one person carrying it all, but about supporting each other through life’s highs and lows.
Conclusion
In the end, I hope my children grow up knowing this truth: that their mama’s greatest strength is not being superhuman but being real.
https://hellotype1.com/en/articles/motherhood-and-type-1-diabetes-why-showing-vulnerability-made-me-a-stronger-mom
Aug 17, 2025 | Healthy Tips

Cervical Cancer
Temitope Adebayo
M.Sc. Industrial Microbiology & Biotechnology | Microbiologist | Research Assistant | Biotech Enthusiast
Introduction
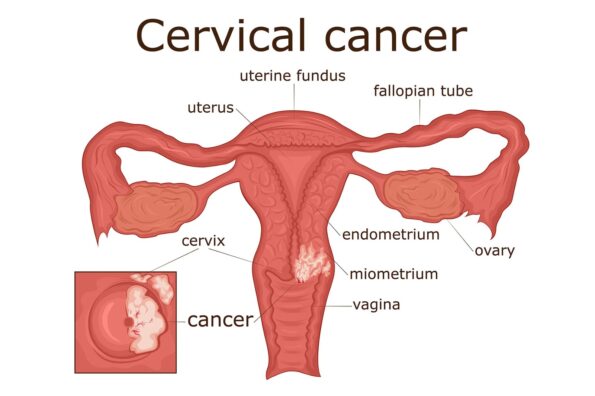
Cervical cancer is a malignant tumour arising from the cells of the cervix — the lower part of the uterus that connects to the vagina. It is one of the most common cancers affecting women worldwide, particularly in low- and middle-income countries. According to global estimates, cervical cancer caused approximately 604,000 new cases and 342,000 deaths in 2020 (WHO, 2022).
Recent years have seen intensified efforts toward elimination. In June 2025, global leaders convened at the second Global Cervical Cancer Elimination Forum in Bali, reaffirming commitments to the WHO’s 90-70-90 targets: 90% HPV vaccination by age 15, 70% screening by ages 35 and 45, and 90% treatment of detected cases. Early detection and prevention are crucial, as the disease is highly preventable and treatable when found in its early stages.
Anatomy and Function of the Cervix
The cervix serves as the gateway between the uterus and vagina. It plays an important role during menstruation, pregnancy, and childbirth. It also produces mucus that changes consistency during the menstrual cycle to either facilitate or block sperm entry.
Causes and Risk Factors
The primary cause of cervical cancer is persistent infection with high-risk types of the human papillomavirus (HPV), especially HPV types 16 and 18, which together account for about 70% of cases (Arbyn et al., 2020). Other risk factors include early onset of sexual activity, multiple sexual partners, smoking, prolonged use of oral contraceptives, a weakened immune system (e.g., HIV infection), and a family history of cervical cancer (CDC, 2023)
Pathophysiology
HPV infects the epithelial cells of the cervix, integrating its DNA into the host genome. This disrupts normal cell cycle control, leading to the production of viral oncoproteins E6 and E7, which inactivate tumour suppressor proteins p53 and Rb. Over time, infected cells may progress from cervical intraepithelial neoplasia (CIN) to invasive carcinoma (Bhatla & Singhal, 2020).
Signs and Symptoms
In its early stages, cervical cancer often produces no noticeable symptoms. As the disease progresses, common signs may include abnormal vaginal bleeding (after intercourse, between periods, or after menopause), foul-smelling vaginal discharge, pelvic pain, and pain during sexual intercourse (WHO, 2022).
Screening and Diagnosis
Routine screening is critical for detecting precancerous changes. Common methods include:
- Pap smear: Detects abnormal cervical cells.
- HPV DNA testing: Identifies high-risk HPV strains.
- Visual inspection with acetic acid (VIA): Used in low-resource settings.
If abnormalities are detected, colposcopy and biopsy are performed for confirmation (Koh et al., 2019).
Staging of Cervical Cancer
The FIGO (International Federation of Gynaecology and Obstetrics) staging system classifies cervical cancer based on tumour size, spread to lymph nodes, and metastasis. Staging helps determine the most appropriate treatment plan (Bhatla & Singhal, 2020).
Treatment Options
- Treatment depends on the stage:
- Early-stage: Surgical removal (conisation, hysterectomy).
- Locally advanced: Radiotherapy with concurrent chemotherapy.
- Advanced stage: Palliative care, targeted therapy, and immunotherapy may be considered (Koh et al., 2019).
Prevention
The most effective preventive measures include:
HPV vaccination: Recommended for girls (and boys) before sexual debut, typically between ages 9 and 14.
Safe sexual practices: Limiting the number of partners and using condoms.
Regular screening: Even vaccinated women should be screened, as vaccines do not cover all HPV strains (WHO, 2022).
Global and Regional Statistics
Cervical cancer remains a major public health issue in sub-Saharan Africa, South-East Asia, and parts of Latin America, where screening programmes are less accessible. The WHO aims to eliminate cervical cancer as a public health problem by achieving 90% HPV vaccination coverage, 70% screening coverage, and 90% treatment for detected disease by 2030 (WHO, 2020).
Challenges in Management
Barriers include limited access to vaccines, screening facilities, and cancer treatment centres in low-resource settings. Cultural beliefs, stigma, and lack of awareness also reduce participation in preventive programmes (Arbyn et al., 2020).
Conclusion
Cervical cancer is both preventable and treatable, yet it continues to claim hundreds of thousands of lives each year. Strengthening HPV vaccination programmes, ensuring regular screening, and improving access to treatment are essential steps toward elimination. Awareness and education remain powerful tools in this fight.
References
1. Arbyn, M., et al. (2020). Estimates of incidence and mortality of cervical cancer in 2018: a worldwide analysis. *The Lancet Global Health*, 8(2), e191–e203.
- Bhatla, N., & Singhal, S. (2020). Primary management of cervical cancer: Society of Gynaecologic Oncology consensus guidelines. *Gynaecologic Oncology*, 157(3), 481–493.
3. CDC. (2023). Cervical Cancer. Retrieved from [https://www.cdc.gov/cancer/cervical](https://www.cdc.gov/cancer/cervical)
4. Koh, W.-J., et al. (2019). Cervical Cancer, Version 3.2019, NCCN Clinical Practice Guidelines in Oncology. *Journal of the National Comprehensive Cancer Network*, 17(1), 64–84.
- WHO. (2020). Global strategy to accelerate the elimination of cervical cancer as a public health problem. World Health Organisation.
6. WHO. (2022). Cervical Cancer Fact Sheet. Retrieved from [https://www.who.int/news-room/fact-sheets/detail/cervical-cancer] (https://www.who.int/news-room/fact-sheets/detail/cervical-cancer)

May 31, 2025 | Healthy Tips


Every year on May 31, the world observes World No Tobacco Day (WNTD), a global initiative led by the World Health Organisation (WHO) to raise awareness about the dangers of tobacco use and advocate for stronger policies to reduce its consumption. This year’s theme, “Unmasking the Appeal”, focuses on the deceptive strategies employed by the tobacco and nicotine industries to attract new users, particularly young people.
As a leading non-communicable diseases (NCDs) support organisation based in Ibadan, Oyo State, Nigeria, Rays of Hope Support Initiative (ROHSI) stands with the global community in amplifying the call for tobacco control, public health protection, and policy enforcement.
The global tobacco epidemic is a formidable threat, claiming over 8 million lives annually worldwide. Of these, more than 7 million deaths are a direct result of tobacco use, while an alarming 1.3 million deaths are due to non-smokers being exposed to second-hand smoke. This exposure is a critical concern for ROHSI, as it also significantly increases the risk of NCDs in non-smokers.
In Nigeria, the situation is alarming:
- 3.4 million Nigerians (2.9% of adults aged 15+) smoke tobacco (2022 data).
- Male smokers (5.4%) far outnumber female smokers (0.4%).
- Tobacco-related diseases – cancer, heart disease, respiratory illnesses, and stroke – place a heavy burden on Nigeria’s healthcare system.
- Economic losses from tobacco-related illnesses and productivity decline further strain families and the nation.
While reports, such as one from the Tribune newspaper, suggest higher smoking prevalence in some northern states, ROHSI emphasises that tobacco use and its link to NCDs is a pressing issue across all regions, including Oyo State.
At ROHSI, we see firsthand the devastating impact of tobacco on individuals and families affected by NCDs here in Ibadan and across Nigeria.
This World No Tobacco Day, under the theme ‘Unmasking the appeal’, we urge a united front to expose the tobacco industry’s tactics that endanger our youth and perpetuate the cycle of NCDs. The first and most crucial step towards a healthier life, free from the threat of many NCDs, is to say NO to tobacco.
ROHSI encourages every Nigerian to reflect on the popular calls to action: “Breathe clean, live green. Quit tobacco today.”
The ROHSI team challenges every individual in Ibadan, Oyo State, and throughout Nigeria to consider making this powerful pledge: “Today, I am pledging to quit all forms of tobacco and nicotine, including cigarettes, smokeless tobacco products, heated tobacco products, e-cigarettes, nicotine pouches, shisha, and other harmful products, for my health and the health of my community.”
Join us in educating others on the dangers of tobacco and industry tactics, support smoke-free policies in workplaces, schools, and public spaces, advocate for stronger tobacco control laws in Nigeria, and help promote cessation programmes through counselling and support.
Together, we can unmask the truth and build a healthier, tobacco-free Nigeria!
About ROHSI:
Rays of Hope Support Initiative (ROHSI) is a Nigerian non-profit organisation based in Ibadan, Oyo State, dedicated to combating non-communicable diseases (NCDs) through awareness, advocacy, and community support programmes.
#NoTobacco #TobaccoFreeGeneration #PublicHealth #WHO_Africa #WorldNoTobaccoDay #ROHSI3 #Nigeria #Africa #Ibadan #NCDs #WHO_Nigeria #WHO_Africa #WHO #TobaccoFree #QuitSmoking #HealthForAll #NNNGO #NCDAlliance #TobaccoFreeNigeria #HealthForAll #FMoH #NPHCDA #NIgerian

Dec 29, 2024 | Healthy Tips

Dear ROHSI Community,
As we embark on a new year, let’s prioritise our health. Non-communicable diseases (NCDs) like hypertension, diabetes, obesity, and high cholesterol are often called “silent killers” because they can develop without noticeable symptoms.
In 2025, we want us all to see the reason why adopting healthy living matters:
Going for early medical screening/detection saves lives: You going for your regular medical checkups is crucial for early detection and management of NCDs, especially hypertension, diabetes, and others.
It helps in adopting preventative measures! Adopting a healthy lifestyle can significantly reduce your risk of developing or worsening these conditions.
Improved Quality of Life! Healthy habits lead to increased energy levels, better sleep, and an overall improved quality of life.
What are the steps to a healthier 2025?
Healthy eating! Focus on a balanced diet rich in fruits, vegetables, whole grains, and lean protein. Limit processed foods, sugary drinks, and excessive salt intake.
Regular Exercise! Aim for at least 150 minutes of moderate intensity exercise most days of the week. You can start with 30 minutes and, with time, increase it to more minutes.
Maintain a Healthy Weight! If you are overweight or obese, consult a healthcare professional for personalised advice on weight management.
Manage your stress! Practicing stress-reducing techniques like meditation, yoga, or spending time in nature, or taking your mind off those activities that can lead to stress, will go a long way in making you healthy.
Regular Checkups! Seat with your medical team, schedule, and attend regular medical checkups, including blood pressure, blood sugar, and cholesterol screenings, among other recommended tests. All towards your wellness
Remember this! Making small, sustainable changes to your lifestyle can have a significant impact on your overall health, and consulting with a healthcare professional for personalised advice and support will go a long way in some of the avoidable health crises that can threaten our health and wellness as we age.
Lastly, always consult with a qualified healthcare professional for any health concerns or before making any decisions regarding your health.
Let’s make 2025 a year of prioritising our health and well-being.
Sincerely,
The ROHSI Management Team

Oct 6, 2024 | Healthy Tips

Every October, World Cerebral Palsy Day unites communities around the globe to raise awareness and promote inclusivity for individuals living with cerebral palsy (CP). This annual event provides an opportunity to shine a light on the challenges faced by those with CP while celebrating their achievements and potential. At cerebralpalsyguidance.com, we are committed to offering resources and support to individuals with cerebral palsy and their families. This article explores the significance of World Cerebral Palsy Day, available support, and how we can all contribute to a more inclusive society.
Understanding Cerebral Palsy
Cerebral palsy is a neurological disorder that affects movement, balance, and posture. It is the most common motor disability in childhood, resulting from abnormal brain development or damage. The effects vary widely among individuals, with some managing to walk independently while others rely on wheelchairs or other assistive devices.
The Significance of World Cerebral Palsy Day
Observed on October 6th, World Cerebral Palsy Day serves as a platform to amplify the voices of individuals with CP and advocate for their rights. The day encourages participation in activities that promote awareness and inclusion, ranging from sharing personal stories to organizing community events. Learn more about global initiatives at the World CP Day official site.
Raising Awareness and Education
Awareness is crucial for fostering understanding and support for individuals with CP. Educating the public can dispel myths and reduce stigma, creating a more inclusive environment. Schools, workplaces, and communities can implement awareness programs to ensure everyone is informed about the challenges and capabilities of individuals with CP. Discover educational resources at Cerebral Palsy Alliance.
Cerebral Palsy and Diabetes
A critical aspect of cerebral palsy is its association with other health conditions, such as diabetes. Studies indicate an increased risk of diabetes in individuals with CP, partly due to reduced mobility and obesity. Furthermore, maternal diabetes has been linked to a higher risk of CP in infants, highlighting the importance of managing diabetes during pregnancy. For more on this connection, visit the Mayo Clinic’s guidance on diabetes and pregnancy.
Support and Resources
Support extends beyond awareness, encompassing access to therapy, educational support, and financial assistance. Therapies like physical, occupational, and speech therapy are vital for skill development and mobility maintenance. Educational support through individualized education programs (IEPs) ensures that children with CP receive tailored learning experiences. Financial assistance is available to help cover medical care, therapy, and adaptive equipment costs. Explore financial assistance options.
Technological Advancements
Innovations in technology have opened new avenues for supporting individuals with CP. Assistive technologies, such as communication devices and adaptive equipment, enhance independence and quality of life. For the latest in assistive technology, visit AbleData’s assistive technology resources.
Community and Advocacy
Building a supportive community is essential for empowering individuals with CP. Advocacy groups and online communities offer platforms for sharing experiences and influencing policy changes. Joining advocacy groups can promote better inclusion and accessibility in society. Check out Cerebral Palsy Foundation’s advocacy efforts.
Celebrating Achievements
World Cerebral Palsy Day is also a time to celebrate the achievements of people with CP. Stories of success and determination inspire others and challenge societal perceptions. Highlighting these achievements honors their hard work and motivates others to pursue their dreams. For inspiring stories, visit Cerebral Palsy News Today’s success stories.
How You Can Get Involved
There are numerous ways to participate in World Cerebral Palsy Day. Whether through volunteering, fundraising, or spreading awareness, your involvement can make a difference. Volunteering at local events or supporting organizations dedicated to CP can amplify their efforts. To find volunteering opportunities, visit VolunteerMatch.
Conclusion
World Cerebral Palsy Day is more than a day of recognition; it’s a call to action for all of us to contribute to a more inclusive and understanding world. By raising awareness, supporting advocacy, and providing resources, we can help those with cerebral palsy lead fulfilling lives. Let us all celebrate this day by embracing diversity and empowering those with cerebral palsy to reach their full potential.
https://www.cerebralpalsyguidance.com/








